OBJECTIVES
In this lecture, we will:
- Discuss how biology affects gender
- Review the genetic blueprint for females and males
- Discuss some of the genetic complications that can occur as they relate to the sex hormones
- Examine what happens when a fetus is exposed to unusual patterns of prenatal hormones
- Review the categories of intersexed individuals
- Discuss and evaluate biologically based theories and the biological influence on the development of gender-typed behaviors
Maria Lavooy, PhD
SCROLL
HORMONES AND CHROMOSOMES
The Genetic Blueprint for Females and Males
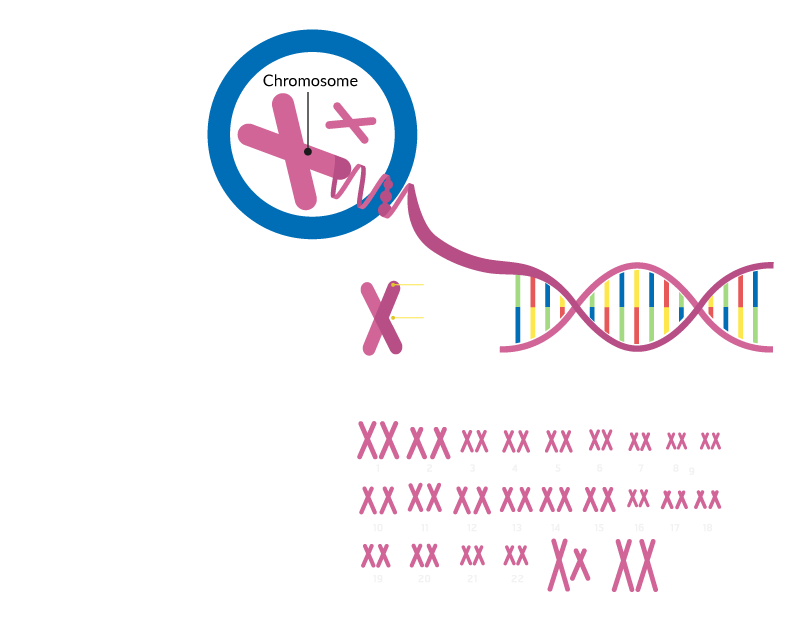
If all goes as it should, a sperm and an egg, or ovum, combine at conception. The new cell, the zygote, contains 23 chromosomes from the father and 23 chromosomes from the mother. There are 22 pairs of autosomes and one pair of sex chromosomes, for a total of 46 chromosomes.
The child will be a genetic female if the zygote contains two X chromosomes – one from the mother and one from the father. The child will be a genetic male if the zygote contains one X chromosome, contributed by the mother, and one Y chromosome, contributed by the father.
Genetic Complications
The X chromosome carries more information than does the Y chromosome. More than 300 X genes have been identified. Fewer than 10 functional Y genes have been identified. There are many genetic complications related to the sex chromosomes. There are sex-linked traits determined by genes on the X chromosome. When combined with the Y chromosome, this can cause disorders typically passed from mother to son.
Females have the extra healthy X to counteract the effects of the X chromosome with the disorder-producing gene. Males do not have the healthy X, as they carry only one X. Therefore, males are more vulnerable to sex-linked disorders such as hemophilia, color blindness, or ocular albinism.
There are other genetic problems that can occur. For example:
- A female with only one X chromosome, referred to as Turner syndrome
- A female with three X chromosomes
- A male with one Y and two X chromosomes
- A male with two Ys and one X chromosome
At least one X is required for the fetus to be viable. A Y alone does not happen in nature.
Genetically Transmitted Syndromes
But what happens if the fetus is exposed to an unusual pattern of prenatal hormones? This may lead to congenital adrenal hyperplasia (CAH) or adrenogenital syndrome (AGS), which are genetically transmitted syndromes. They cause the adrenal glands of the fetus to malfunction. There is a release of excess androgens (the male hormones) from the prenatal period on.
Select each term to learn more about other genetically transmitted syndromes.
This would suggest that biology is responsible for gender identity, but the results are not so clear cut. Upon closer examination, it was found that the transitions these individuals made from identifying with one gender to identifying with another were not smooth. While biology was certainly important in influencing their gender identification, the culture of these individuals was also important.
This results in a female – masculinized genitalia but internally still a female. Behaviorally, in terms of sex-typed activity and preferences, CAH girls are somewhere between non-CAH girls and typical boys. However, the outcome and extent of this condition depend on the amount of the androgen substance (or hormone) that enters the fetus’s bloodstream and the time at which the entry occurs.
This occurs in an individual with an XY chromosomal pattern (that should mean male) that is insensitive to prenatal androgens (the male hormones). The genetic blueprint is male, but remember, male development needs the secretion of male hormones.
If the fetus is insensitive to these androgens, or male hormones, the result is that the individual may have female or ambiguous external genitalia.
This is a recessive genetic disorder wherein an XY individual develops a normal internal reproductive system, but due to a deficiency of the steroid 5-Alpha reductase, the external genitalia do not develop. The individual appears female until the testes begin to produce testosterone during adolescence, which results in the development of masculine secondary sex characteristics, including a penis and scrotum.
These individuals are raised all through childhood and into adolescence as females. However, early reports indicated that they quite easily adopted the male identity at puberty.
summary
In this lecture, we:
- Discussed how biology affects gender
- Reviewed the genetic blueprint for females and males
- Discussed some of the genetic complications that can occur as they relate to the sex chromosomes
- Examined what happens when the fetus is exposed to unusual patterns of prenatal hormones
- Reviewed the categories of intersexed individuals
Stock images provided by Thinkstock.